
“After I receive this double lung transplant I hope just the everyday living tasks are a lot easier. Just being able to spending my life making countless memories with my children without the struggle to breathe.” Stephanie is a 32 year old Cystic Fibrosis (CF) patient who is in need of a double lung transplant. She was diagnosed with CF when she was 6 weeks old and has had many complications along the way. Stephanie was an athlete and dancer during her childhood. Her active lifestyle kept her CF symptoms at bay for most of her school years. However, when she was a senior in high school, she was hospitalized for the first time. After high school her CF continued to worsen especially after she became pregnant with her first child at 22. The weight she gained from her first pregnancy made it difficult for her lungs to function properly. Her second pregnancy made her life even more difficult. Although she had two healthy children without CF, her health took a turn for the worse. Stephanie is now raising her two children with only 20% lung function. Everyday tasks like playing with her children are extremely difficult for her and she spends much of her time taking breathing treatments during the day. She also stopped working at her job as a medical billing and coder and give up many hobbies such as swimming, traveling, and dancing. In 2018 alone she has been hospitalized 5 times. She was put on oxygen 24/7 and on a feeding tube to help her gain weight. Following her last serious hospitalization episode, her doctors began the process of getting her ready for a double lung transplant. Without it, they said, she has about two more years to live. Despite all of the hardships, Stephanie is hopeful about the future. “After I receive this double lung transplant I hope just the everyday living tasks are a lot easier. Just being able to spending my life making countless memories with my children without the struggle to breathe.” She also has some inspiring words and advice for others living with CF. “I’d just like to let anyone who is fighting this disease [know] to never give up [and] always have hope. I have beaten the odds past my life expectancy of 18, [and] was told I couldn’t conceive or even birth a child. I’m very blessed with two very healthy cystic fibrosis free kids. Never let anyone tell you that you won’t or can’t. Believe in yourself and just keep fighting!” Stephanie plans to use the funds donated for medical bills her insurance doesn’t cover such as co-pays and other post-transplant care. You can help Stephanie on her road to a double lung transplant by donating here:
0 Comments
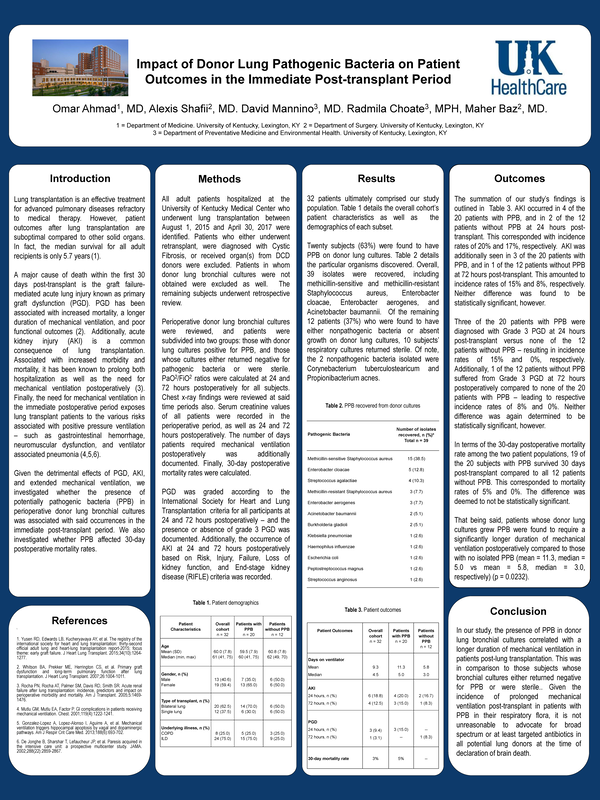
The Sid Foundation donated $3000 to the University of Kentucky Hospital Lung Transplant Program at the end of 2017 to fund lung transplant research. Here is the research we funded: Here is a summary of the research written by the UK Healthcare team: "The generous gift from the Sid Foundation was used in two parts. First, funds were used to support research investigating the correlation between bacteria and organ rejection in post-lung transplant patients. Their research revealed a greater need for broad spectrum antibiotics at the time of donor brain death in order to limit harmful, life threatening bacteria and increase survival rates among lung transplant patients. Tangential research will allow for more advocacy in this arena, with the ultimate goal of limiting pathogenic bacteria and improving the life span of lung transplant patients. This research was presented at the International Society for Heart and Lung Transplantation in Niece, France. The investigators presented the attached poster. An abstract is below. Impact of Donor Lung Pathogenic Bacteria on Patient Outcomes in the Immediate Post-transplant Period Abstract: Lung transplantation is an effective treatment for advanced pulmonary diseases refractory to medical therapy. However, patient outcomes after lung transplantation are suboptimal compared to other solid organs. In fact, the median survival for all adult recipients is only 5.7 years. A major cause of death within the first 30 days post-transplant is the graft failure-mediated acute lung injury known as primary graft dysfunction (PGD). PGD has been associated with increased mortality, a longer duration of mechanical ventilation, and poor functional outcomes. Additionally, acute kidney injury (AKI) is a common consequence of lung transplantation. Associated with increased morbidity and mortality, it has been known to prolong both hospitalization as well as the need for mechanical ventilation postoperatively). Finally, the need for mechanical ventilation in the immediate postoperative period exposes lung transplant patients to the various risks associated with positive pressure ventilation – such as gastrointestinal hemorrhage, neuromuscular dysfunction, and ventilator associated pneumonia. Given the detrimental effects of PGD, AKI, and extended mechanical ventilation, we investigated whether the presence of potentially pathogenic bacteria (PPB) in perioperative donor lung bronchial cultures was associated with said occurrences in the immediate post-transplant period. We also investigated whether PPB affected 30-day postoperative mortality rates." If this still sounds too complicated to understand, don't worry. Your donations are helping increase the survival rate of lung transplant patients by funding lung transplant research.
Thank you for your donations! To help us keep growing, click here. |


 RSS Feed
RSS Feed