|
We are deeply saddened by the state of our country right now.
As a nonprofit, our work is always to help those who are underserved or those whose voices are unheard in the community. In the last five years, despite meeting and getting to know many lung transplant patients, we couldn’t help but notice the lack of diversity in people who are able to get a lung transplant in this country. It is because of economic and racial inequality in the United States that many people of color do not have access to the healthcare system. This means that there are many people of color who have lung diseases and need lung transplants, but cannot afford to see a doctor or get a transplant because of a lack of health insurance or funding. Because of this disparity, we have been able to help very few people of color who need lung transplants. They often just don’t have the resources to get one. Our goal for the near future is to continue to build ourselves and raise more funds so that we can not only financially assist lung transplant patients who are already on their way to getting a transplant, but also have the resources and funding to help more people of color who may not even get the opportunity to see a doctor about their lung health issues and help them pay for an entire transplant. The state of our country is especially grave right now. Again, due to racial inequality, COVID-19 has been disproportionately killing Black and Indigenous Americans. On top of that, today police brutality is one of the leading causes of deaths for Black males in America. The combination of COVID-19 and racial inequality affects lung transplant patients of color in more devastating ways than white lung transplant patients and makes their survival much more difficult. In addition to lung transplants being expensive, over half of lung transplant patients do not live more than 5 years post transplant. These odds of survival are lessened even more for transplant patients of color due to the factors I mentioned earlier. We stand in solidarity with our Black lung transplant patients as well as Black Americans with lung health issues. We stand in solidarity with all Black Americans during this difficult time. We hope to continue to grow our small nonprofit to serve your needs more efficiently in the near future. I am the President of The Sid Foundation and am a woman of color. Although nonprofits like ours (run by POC) are statistically doomed to fail within the first couple of years and do not receive as much funding as nonprofits run by white board members and administrators, we are going to continue to beat the odds to serve our community. Due to COVID-19, our organization has taken a huge hit financially. We are not stopping our work, however, and will continue to keep moving forward until we see better times. We hope that our immunocompromised transplant patients have the ability to stay home and stay safe. If not, we hope that you have access to protective gear to keep yourself as safe as possible. To our supporters who are not immunocompromised, please keep transplant patients and anyone else that might be immunocompromised in your thoughts as you go about your daily activities to make sure you are making the environment safer for them. Here are some resources that you can use to help you stay safe during these times. You can also donate to these organizations to help others stay safe: The World Health Organization The National Healthcare for the Homeless Council The American Civil Liberties Union Black Lives Matter The Minnesota Freedom Fund
0 Comments
This month is The Sid Foundation’s 5 year anniversary! Over the last 5 years, we’ve raised more than $50,000 to support lung transplant research and patients. We’ve also published three Lung Girl comic books, created tons of educational content online, and hosted several community events. We couldn’t have done all of this without your help! A huge thank you to our corporate sponsors: Our recurring individual donors: Damini Mathur Alka Vahal Rakesh Vahal Gaurav Mathur Sonu Sachdev And all individual donors (see list here) for helping us grow throughout the years! Also, thank you to all of you who purchased a comic book, t-shirt, or other merchandise from us. We are so grateful for all your support and hope to continue to make you proud to sponsor our work. The Sid Foundation was established one year after my brother Sid Vahal passed away due to complications from his double lung transplant. My family and I have been on a mission to try our best to help anyone else in Sid’s shoes. It has been a privilege to be able to help so many lung transplant patients over the last five years with your undying support. Since we can’t have a party and thank you in person due to COVID-19, here’s a video of me expressing my gratitude: As the entire world continues to stay locked down during the COVID-19 epidemic, we want to bring attention to how this situation affects lung transplant patients and medical staff. As you may or may not know, transplant patients have a compromised immune system. This means that their body has a much more difficult time fighting illness. The Coronavirus can be fatal to people with compromised immune systems. People with compromised immune systems don’t necessarily look “sick” or “weak” so it is important for all of us to be careful who we are around during this time.
The following people have a weak or compromised immune system:
These are the people that have the highest risk of dying from COVID-19. You most likely know someone who is immunocompromised. This is why social distancing and self-quarantine is so important. You might be healthy and able to fight off the Coronavirus, however, your family and friends may not be able to. We also want to bring attention to all the healthcare workers like doctors, nurses, techs, administrative staff, and all others who are on the frontlines of this epidemic. They are putting their lives at risk to help save ours. Hospitals are at capacity with people fighting COVID-19. Please help make their job easier by keeping yourself as safe as possible in this epidemic. Everyone does not have the privilege of staying home, especially those with essential jobs like healthcare workers, delivery people, and some retail workers. For those that do have the choice, please stay home. Although there is no need to panic and buy things like toilet paper in bulk, it is important to stay as vigilant as possible. We can all play a part in slowing down this epidemic and saving the lives of those people that are most vulnerable by following the guidelines of the World Health Organization. Make sure to wash your hands as often as possible and avoid crowded places. Also, consider checking up on the people in your life that might have a compromised immune system to make sure they are safe and have everything they need. We hope all of our family, friends, donors, supporters, and lung transplant patients stay safe during these difficult times. If you have the means, please donate to the WHO and other accredited organizations that are helping us fight this. Stay safe!
Thank you to everyone who helped us raise funds for Nicole Fournier!
Because of your donations we were able to raise $300 to help Nicole begin her new life. How Will Your Donations Help Nicole? Nicole has had to relocate due to her lung transplant surgery. These funds will help her with living costs and/or medical bills related to her transplant. Lung transplants have the lowest survival rate of all organ transplants, so your donations are helping Nicole beat the odds and live a longer healthier life with her new lungs. About Nicole To read more about Nicole’s journey click here. Donations If you haven't donated to Nicole’s fundraiser yet, it's not too late! Donate here: 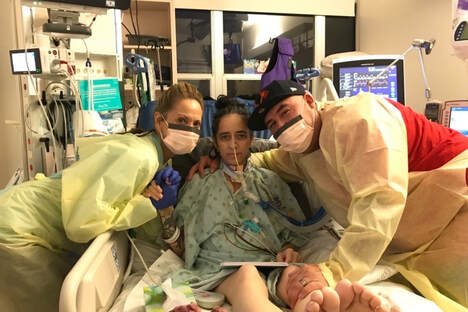
"Most people know I have CF [Cystic Fibrosis] but no one knows what I really go through." - Nicole
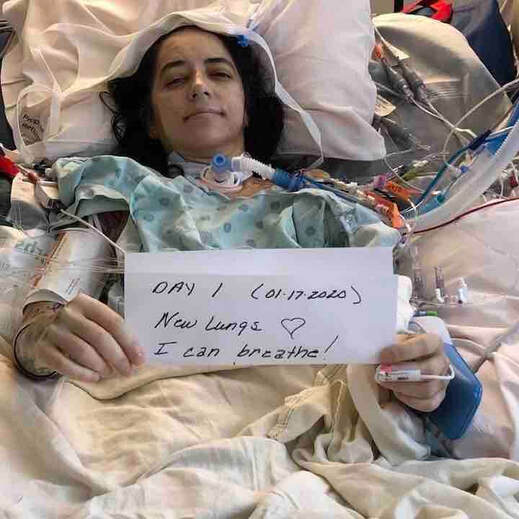
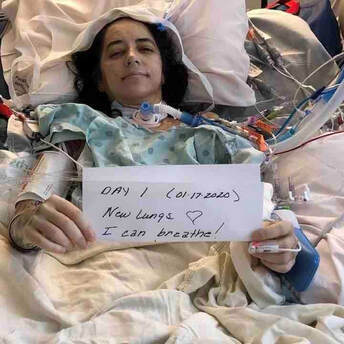
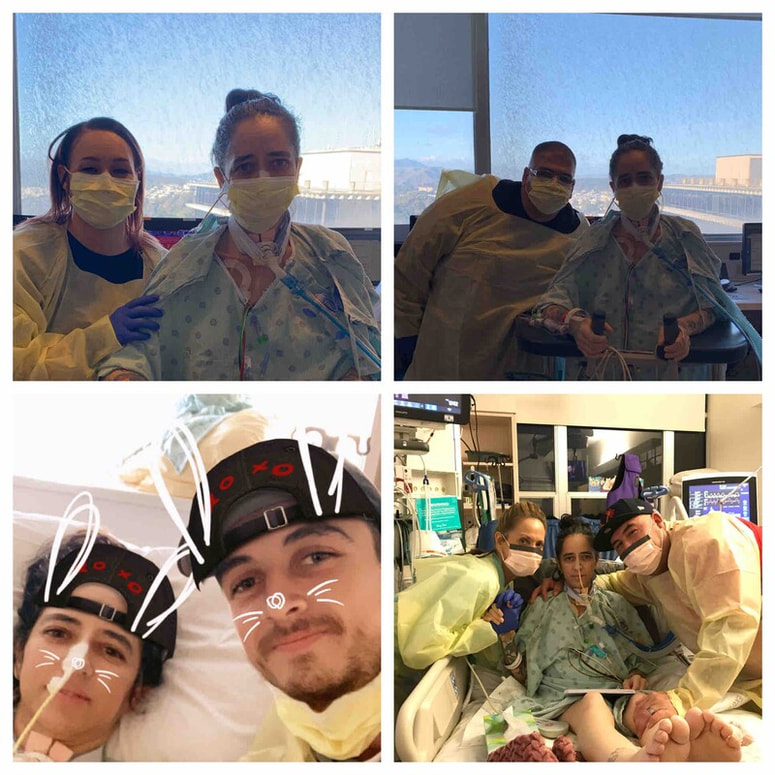
Nicole is a 41 year old woman from Sacremento, CA who has lived with Cystic Fibrosis (CF) her whole life. She is a wife and a mother of two. Her hobbies include spending time with family, taking her dogs out for a walk, shopping, taking road trips, and watching T.V. Unfortunately, she is unable to do any of these things right now because she is in the hospital. Nicole was born with Cystic Fibrosis, a genetic lung disease with no cure. "She quickly learned to push on, regardless of how bad she was feeling. She also learned to accept this constant illness as 'normal.'” - Nicole’s mother. Although she was often sick as a child, she wasn’t diagnosed with CF until she was 19 years old and pregnant. Not only did she have a scary pregnancy, but she also found out that CF was a lifelong disease without a cure. In fact, today, the average lifespan of a person with CF is into the late 30s to early 40s. Although Nicole had already begun the process of being evaluated for a lung transplant due to her declining health, on December 27th, she had to be rushed to the hospital because of a severe lung infection. Her condition was so unstable, that on January 7th, doctors told Nicole’s family that she only had a few hours to live and they should say their goodbyes. Her family was not ready to give up, however. Nicole was moved from UC Davis hospital to UCSF. On January 12th the doctors here were able to stabilize her condition and put her on the list to receive a double lung transplant. Five days later on January 17th, Nicole’s doctors found a donor and performed her double lung transplant. She was lucky to be able to find a donor so quickly. Nicole can now breathe on her own. She is recovering from her lung transplant surgery in the hospital. Although she will no longer need to carry around oxygen with her wherever she goes, living with a lung transplant is similar to living with CF in that she will still need to take around 50 pills a day to keep her body from rejecting her new lungs and to keep all her other organs running smoothly. Lung transplants also have the lowest survival rate of all organ transplants. Only about 50% of patients live five years past the transplant. Nicole has traded one disease for another. She still has a difficult road to recovery ahead of her. Nicole and her husband Bobby have been unable to work because of her hospitalization. They will now need to move to San Francisco and live within a 30 minute drive of the hospital for at least the next 3 months so she can have regular check ups. This means that in addition to medical bills, Nicole will have new living costs which include housing, food, gas, and more while in San Francisco. Despite the challenges, Nicole is hopeful and grateful. “I’m so grateful for my donor and this second chance at life.” - Nicole Once Nicole has recovered and is able to live a more normal life, she plans to go hiking, taking walks on the beach, climb stairs, walk in the mall, go to the grocery store, and just enjoy life. “She loves her life and is grateful for each new day. Not only is she beautiful, she has a playful spirit, and a strong will. She has a proven strength and determination that not many people possess. In a word, she is a fighter. She loves her life, her two boys, her friends, family, pets, and her best friend/love of her life and constant companion Bobby.” - Nicole’s mother Her advice for others with CF or other lung disease who might need a lung transplant one day is: “Fundraise as much as possible even if you have not been listed yet. Reach out to places for help and donations. It’s very hard to heal when you are so worried about how you are going to pay for everything.” Living with CF or any other lung disease without a cure can be scary. Getting a double lung transplant can be scary too. Nicole is an inspiration for many with how hard she has been fighting to live through her disease and now after her lung transplant. Please help Nicole and her family continue to fight by donating today. You donation will be used for medical bills, relocation costs, living expenses, transportation expenses, and any other expenses that might arise while Nicole is recovering. “My mother is not a person to ever ask for help... Anything will help, I just want my mom to enjoy life and have a second chance without the worry of bills and expenses.” - Nicole’s son, Austin.
To help Nicole beat the odds and live a long and healthy life after her transplant, please donate here:
2019 was a busy year for us. We accomplished many of the goals we set and much more!
2019 Accomplishments: 1.) Donated $5000 to the University of Kentucky Hospital Lung Transplant Program - $3000 funded lung transplant research - $2000 helped lung transplant patients pay for medication 2.) Began our “care package” program: sent out 20 care packages for lung transplant patients throughout the year. Learn more about our Lung Transplant Patient Support Program here. 3.) Received the Google Ad Grants. Learn more about it on this blog. 4.) Revamped our website. 5.) Published Lung Girl #3 in October. Purchase the latest comic in the Lung Girl comics series here. 6.) Created tons of new educational content about lung diseases like asthma and COPD. Check out our previous blogs to learn more. 7.) Increased our donors. We could not have accomplished all of this without your support. Thank you! We are also excited to work on our goals for 2020! 2020 Goals: 1.) Continue to donate to the University of Kentucky Hospital Lung Transplant program. We will continue to fund their lung transplant research and provide funds to help their lung transplant patients pay medical bills. 2.) Have more fundraisers for lung transplant patients. 3.) Send out more care packages to lung transplant patients. 4.) Increase our community outreach even more through online platforms. 5.) Create more educational content about lung health and lung diseases. 6.) Apply for and obtain more grants to help us increase our revenue. 7.) Increase individual and corporate donors. Again thank you to our individual donors and corporate donors who have made this possible. We have been successfully growing for almost 5 years because of your support! If you would like to keep supporting us, donate now:
Donate Now
It seems the holiday season begins earlier every year, but the frenzy of shopping truly launches the day after Thanksgiving - commonly known as Black Friday.
As more and more people began to turn to online shopping, Cyber Monday emerged, too. Although all this shopping is done in the name of giving gifts to loved ones, it sometimes feels like the goodwill of the holiday season fades into the background. In 2012, a few nonprofit professionals decided to do something about it. Several organizations joined forces to create the first annual Giving Tuesday. Over 2,500 social impact organizations participated in the inaugural event, raising more than $10 million. But Giving Tuesday was just getting started. In 2013, the number of participating organizations quadrupled and donations nearly doubled. In 2014, more than 20,000 organizations raised $45.7 million. and in 2015, $116.7 million was raised. And 2017, the giving day raised over $177 million online. The Sid Foundation would love to partner with you for Giving Tuesday! Every dollar you donate will be a direct step toward saving lung transplant patients.
COPD and Asthma? What's the difference. How do I know I have COPD or Asthma? In this blog post we will compare and contrast COPD and Asthma so you have a better understanding of which is which.
COPD is a chronic lung ailment due to which the patient will feel difficulty to breathe since the lung airflow is affected. The symptoms of COPD are shortness of breath, coughing and clearing throat. COPD is irreversible and the causes of COPD are smoking and continued exposure to dust, harmful gases, chemicals and other air pollutants. Asthma is a respiratory condition marked by spasms of bronchi. Due to the inflammation the airways in the lungs become narrow. Asthma leads to breathing difficulty as a result of an allergic reaction. Asthma will cause shortness of breath, wheezing and chest tightness. Asthma can be reversed by taking medical treatment and the patient can be back to normal breathing. Various substances can trigger asthma attacks. Similar signs and symptoms When we consider COPD Vs Asthma it is to be noted that there are a few common signs and symptoms – cough, shortness of breath, chest tightness, anxiety, wheezing and intolerance. JOIN 200+ DONORS WHO'VE DONATED OVER $40,000 TO HELP LUNG TRANSPLANT PATIENTS. DONATE WHAT YOU THINK IS FAIR. MOST PEOPLE DONATE AT LEAST $10Different signs and symptoms In case of COPD, the breathing never returns to normal whereas in case of asthma the breathing returns to normal between attacks. COPD symptoms become more severe gradually whereas in the case of asthma the symptoms may or may not become severe. When compared to asthma, COPD will produce more mucus and phlegm. COPD will cause chronic cough and chronic blueness of lips and fingernail beds. This will not happen in the case of asthma. A person of any age can be affected by asthma whereas COPD normally occurs in those who are above 40 years. Causes: COPD Vs Asthma COPD is caused either by cigarette smoking or lung irritants including toxic fumes, chemicals and dust that cause damage of lung cells. Both cigarette smoke and tobacco-smoke cause COPD. Inherited genetic factors such as alpha- 1 antitrypsin deficiency also cause COPD. The main cause of asthma is the immune reactions to asthma triggers that take place in the airways causing inflammation. Asthma gets triggered by cigarette smoking also. However, asthma triggers differ from patient to patient. The most common asthma triggers are airborne substances such as pollen, mites, dust, mold, pet dander and various other substances. Treatment: COPD Vs Asthma The use of combined bronchodialators is the most widely accepted treatment for COPD. COPD patients can take vaccinations to reduce the risk of respiratory-track infections. Those who smoke are asked to get rid of the habit completely. Oxygen therapy can improve the survival of COPD patients. In the case of asthma, the doctor will discuss with the patient and will recommend the best treatment and the most suitable drugs. Medications include corticosteroids and short acting beta agonists. When exacerbations become severe, anticholinergic medications will be provided. In case the patient is desensitized to certain asthma triggers allergy shots will be prescribed by the doctor. Emergency treatment for both COPD and Asthma involves intravenous corticosteroids, incubation, mechanical ventilation and oxygen treatment. Prognosis and life expectancy: COPD Vs Asthma In case of COPD prognosis will be from fair to poor and depends on how fast the disease advances over time. Generally, lifespan of COPD patients decreases. Prognosis for asthma is from fair to excellent. It depends on how well the patient identifies his/her triggers and his/her response to the medication. Conclusion According to WHO estimates, 65 million people have moderate to severe chronic obstructive pulmonary disease (COPD). More than 3 million people died of COPD in 2005, which corresponds to 5% of all deaths globally. Severe COPD can get to a point where your lungs may stop functioning and you may need a lung transplant. Did you know that lung transplants have the lowest survival rate among all transplants? Only about 50% of people live 5 years after having a lung transplant and patients have to take up to 50 pills a day! We at The Sid Foundation want to increase that survival rate and help patients be able to afford that medication which is why we raise money for lung transplant research and development and lung transplant patients. We need your help in increasing the survival rate and helping lung transplant patients so please join the 200+ donors who have raised over $40,000 and donate what you think is fair to help lung patients everywhere. If you donate $10 or more, we will send you a free Lung Girl comic book and put your name on our wall of donors so that you can be recognized for your contribution forever.
Chronic obstructive pulmonary disease (COPD) is an inflammatory lung ailment which will cause obstruction of airflow to and from the lungs. Apart from cigarette smoking, other causes for COPD include prolonged exposure to harmful gases, dust, chemicals or other air pollutants. Those who are affected by COPD are more vulnerable to lung cancer and cardiac ailments. The two most common lung ailments - chronic bronchitis and emphysema - can lead to COPD.
Daily cough and production of sputum are the signs of chronic bronchitis. Air passes through the bronchial tubes to and from the air sacs of the lungs which are also known as alveoli. Inflammation of the lining of the bronchial tubes is called chronic bronchitis. Alveoli are the smallest air passages of the lungs and when the alveoli are destroyed as a result of cigarette smoking or exposure to irritant gases or air pollutants, the condition is called emphysema. COPD can be treated and if detected earlier, treated properly and managed correctly, those affected by this disease can control the symptoms to a great extent and lead a comfortable life. Proper treatment, as well as managing of COPD, is essential to avoid the risk of associated conditions. Here are a list of Signs and Symptoms of COPD JOIN 200+ DONORS WHO'VE DONATED OVER $40,000 TO HELP LUNG TRANSPLANT PATIENTS. DONATE WHAT YOU THINK IS FAIR. MOST PEOPLE DONATE AT LEAST $10Symptoms and signs Difficulty in breathing, wheezing, and production of sputum are considered as basic symptoms of COPD. Exposure to smoking or air pollutants is the main cause of COPD and if the exposure continues for a long period of time the disease is likely to worsen. In most of the cases, by the time the symptoms of COPD appear it might have inflicted considerable damage to the lungs. If a person has daily cough and production of sputum for no less than three months in a year for two consecutive years it can be taken as a symptom of chronic bronchitis. Those affected by COPD will experience shortness of breath, especially during physical activities. Wheezing and tightness of chest also indicate COPD. There will be an excessive quantity of mucus in the lungs of those affected by COPD and as a result, COPD patients have to clear their throat daily in the morning. Chronic cough and production of clear, white, yellow or green sputum are also signs of COPD. If the lips and fingernail beds get bluish, it is to be taken as a sign of COPD. This phenomenon is called cyanosis. COPD patients are prone to frequent infections of the respiratory system. The patient will experience a lack of energy and may also experience gradual weight loss. Swelling of ankles, legs, and feet is also a sign of COPD. The symptoms of COPD may get worse for a few days and such episodes are called exacerbations. If you have been seeing any of these symptoms lately please talk to your doctor to see if you have COPD. The earlier it is detected and the faster it is treated the better and more comfortable life you will have. Conclusion According to WHO estimates, 65 million people have moderate to severe chronic obstructive pulmonary disease (COPD). More than 3 million people died of COPD in 2005, which corresponds to 5% of all deaths globally. Severe COPD can get to a point where your lungs may stop functioning and you may need a lung transplant. Did you know that lung transplants have the lowest survival rate among all transplants? Only about 50% of people live 5 years after having a lung transplant and patients have to take up to 50 pills a day! We at The Sid Foundation want to increase that survival rate and help patients be able to afford that medication which is why we raise money for lung transplant research and development and lung transplant patients. We need your help in increasing the survival rate and helping lung transplant patients so please join the 200+ donors who have raised over $40,000 and donate what you think is fair to help lung patients everywhere. If you donate $10 or more, we will send you a free Lung Girl comic book and put your name on our wall of donors so that you can be recognized for your contribution forever.
There are various COPD stages. Determining the right stage of the disease is a must, so that the proper form, mode, and intensity of treatment can be determined. Medications, lifestyle changes, the tools, and accessories used for keeping symptoms under control; all are decided upon the detection of the stage of COPD.
Spirometry test determines COPD stages There is a proper test to determine what stage the disease is in. This test is called the Spirometry test. A grading obtained through the test tells the COPD stages. There is a grading system called the GOLD classification under the Spirometry test, which exactly pinpoints the stage of COPD as follows:
JOIN 200+ DONORS WHO'VE DONATED OVER $40,000 TO HELP LUNG TRANSPLANT PATIENTS. DONATE WHAT YOU THINK IS FAIR. MOST PEOPLE DONATE AT LEAST $10Problems from advancing COPD stages With advancing stages of the disease the following problems get aggravated:
How the disease progresses with the stages In the mild stage, the shortness of breath is felt but often ignored. At times the patient would not really notice anything significant other than coughing and expulsion of some mucus at times. Not all patients understand the problem in this stage; however, the lungs get affected inside. In the moderate stage, the problem with breathing worsens and gets noticeable. Patients would notice breathlessness after any brisk activity or even after any normal activity. This is the time when most patients start noticing that they have this problem with breathing and that they are getting less oxygen and are fatigued often. In the severe stage, the airflow to and from the lungs is poor, and shortness of breath is too much. The patient won’t be able to do normal exercises at this point. At times symptoms get too serious which is referred to as exacerbation. The very severe stage comes with life quality getting poor due to very limited airflow, frequent symptom attacks, and extreme difficulty in breathing. Conclusion According to WHO estimates, 65 million people have moderate to severe chronic obstructive pulmonary disease (COPD). More than 3 million people died of COPD in 2005, which corresponds to 5% of all deaths globally. Severe COPD can get to a point where your lungs may stop functioning and you may need a lung transplant. Did you know that lung transplants have the lowest survival rate among all transplants? Only about 50% of people live 5 years after having a lung transplant and patients have to take up to 50 pills a day! We at The Sid Foundation want to increase that survival rate and help patients be able to afford that medication which is why we raise money for lung transplant research and development and lung transplant patients. We need your help in increasing the survival rate and helping lung transplant patients so please join the 200+ donors who have raised over $40,000 and donate what you think is fair to help lung patients everywhere. If you donate $10 or more, we will send you a free Lung Girl comic book and put your name on our wall of donors so that you can be recognized for your contribution forever. |
















 RSS Feed
RSS Feed